Shoulder arthritis causes pain, stiffness and loss of function. When this begins to interfere with quality of life, sleep and
leisure time activity, shoulder replacement is an option to regain comfort and function. As the cartilage between the ball and socket wears away, the bone-on-bone grinding can lead to erosion of the socket’s back wall, allowing the ball to slide out the back or subluxate. As this process progresses, the socket orientation is altered relative to the shoulder blade. This is called
retroversion which essentially means tilting backward. The figure to the right demonstrates this tilting in the B2 example where the head is resting not in the center, but on the back rim. This is a common feature of arthritic shoulders that must be corrected during shoulder replacement in order to guarantee restoring native anatomy to optimize shoulder function after surgery.
Studies have shown that, even in expert hands, the ability of a shoulder surgeon to accurately restore socket orientation though bone preparation and implant choice is imperfect at best. Leaving the artificial socket in too much retroversion can lead to early and mid-term failure of shoulder replacements and potentially alter range of motion after surgery. Fortunately, modern technology can improve surgeons’ accuracy in implant selection and placement using a combination of 3D imaging technology, preoperative planning and intraoperative surgical navigation.
Dr. Moby Parsons has been involved in the design of one such system with Exactech, Inc., a shoulder replacement implant
company located in Gainesville, FL. As part of an international design team (pictured here) including surgeons and engineers from both the United States and France, Dr. Parsons has done extensive research and development to bring the GPS system to market and to Portsmouth Regional Hospital, the only hospital in the state to offer this revolutionary advancement in shoulder replacement.
GPS starts with a CT scan of the shoulder. This provides an exact replica of what each patients arthritic shoulder looks like. This scan is then imported into a preoperative planning software which allows the surgeon to virtually implant the properly selected socket prosthesis in the exact position and orientation that will best restore native anatomy, minimize bone loss and ensure solid fixation in the bone of the shoulder socket. This plan can then be taken to the operating room where the surgeon can use “intelligent” instruments with infrared trackers to navigate the surgery and replicate the plan with great accuracy. This is called navigation. The picture below demonstrates the workflow to the GPS procedure.
In the operating room, the surgeon has a computer mounted to the table which shows in real time how the bone should be prepared in order to ensure proper implant placement. Through a process called registration, boney landmarks are selected with probe that tells the computer where the patients shoulder socket is in space. Instruments used during the preparation including reamers and drills can be directed in real time on the computer screen to ensure that the implant is then placed exactly according to the plan. This essentially gives the surgeon x-ray vision during the case. The pictures to the left shows the preoperative plan for a specific patients arthritic shoulder. To the right and below is the navigation showing how the drill and reamers should be placed and angled to ensure proper position of the implant. GPS is the only current system to allow live navigation of the implant placement.
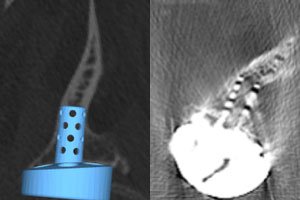
The consequences of improper implant placement are well documented in the shoulder literature with higher early failure of the implant through wear and loosening. GPS technology ensures better mechanics and implant fixation, particularly in more challenging cases where there is advanced wear. The example below shows a patient with a very narrowing glenoid vault who is undergoing a reverse shoulder replacement. As one can see, there is no room for error in the placement of the central post of the baseplate. The postoperative CT scan shows perfect placement. To achieve this without planning and navigation would purely a stroke of luck, something that neither surgeons or patients want to rely on when performing an operation where accuracy matters.
The Knee, Hip and Shoulder Center is proud to offer this technology with an expert design surgeon who has helped to develop and refine the system and validate it effectiveness. Dr. Parsons continues to work extensively on this platform which will bring new features in the future allowing range of motion modeling and better correlation of implant position with patient outcomes. Dr. Parsons recently moderated a panel at the New England Shoulder and Elbow Surgeons Annual Meeting on preoperative planning in shoulder replacement, hosting an international expert faculty in a discussion about the value of these advancements in shoulder replacement. Dr. Parsons work will be featured in several peer-reviewed publications and podium presentations at national and international meetings.
To learn more about our shoulder replacement options, click here.