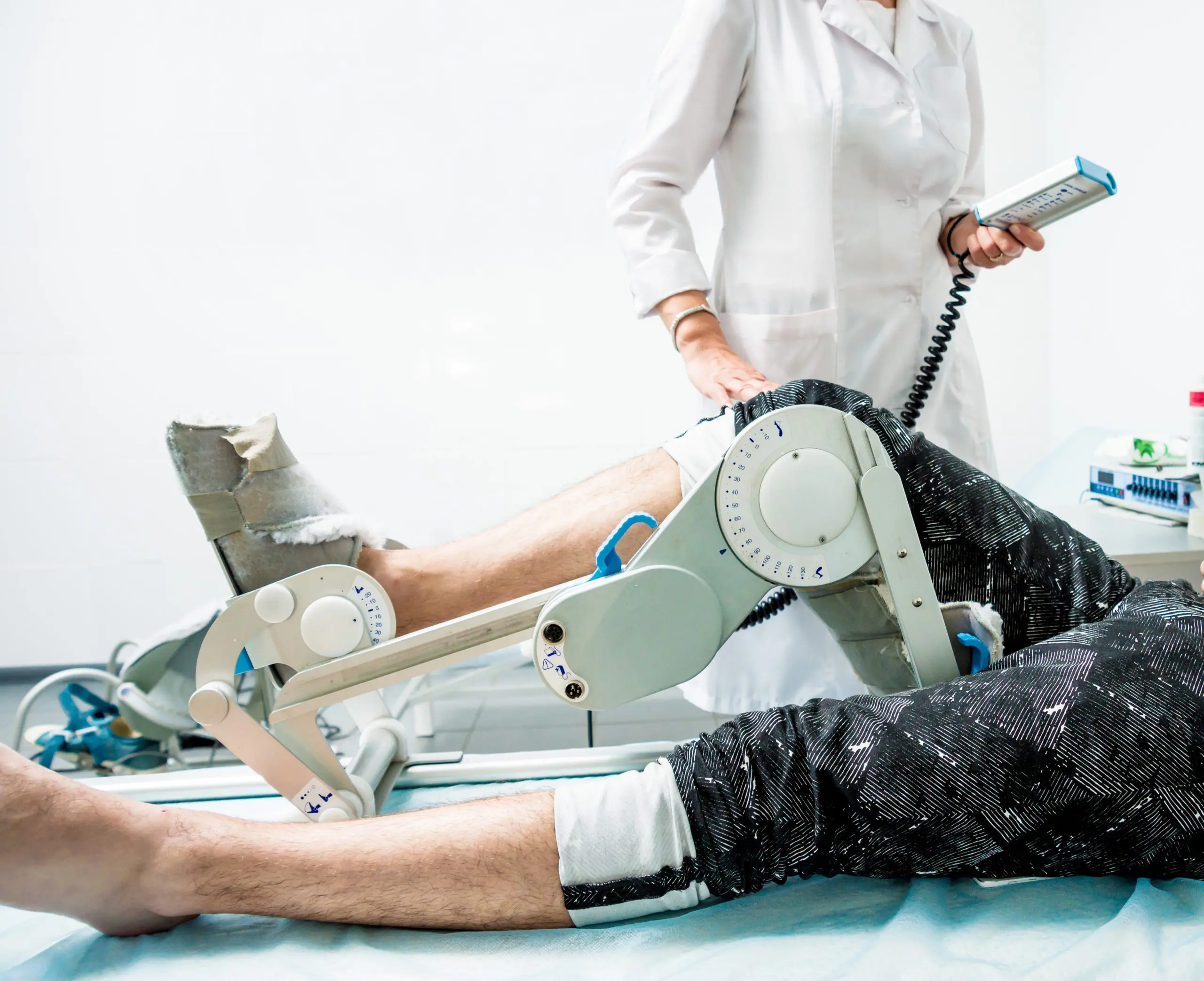
While most knee replacement surgeons have abandoned the CPM, we have embraced it. We have invented solutions for our patients that lead to less pain, a faster recovery and superior outcomes.
The Continuous Passive Motion (CPM) machine was once considered to be the gold standard of post-operative care following total knee replacement surgeries. Originally introduced by Salter, the concept was based on the observation that animal limbs subjected to full arc motion, from complete extension to full flexion for 24 hours a day over a two-week period, experienced accelerated healing, diminished scarring, and enhanced functionality. The fundamental rationale was straightforward: by averting stiffness during the healing process, the limb would be less prone to develop scar tissue that could impede motion.
Nonetheless, when the CPM concept was adapted for human patients, several challenges emerged. The primary issue was the intense pain endured by patients, which the available opioid-based pain relief regimens could not sufficiently mitigate. Although high-dose opioids effectively diminished pain, they also hampered a patient’s ability to engage in rehabilitation due to respiratory depression. Surgeons were also concerned that flexing a knee with a wound closed while the knee was straight might cause the wound to rupture. Consequently, most protocols postponed the introduction of the CPM machine, restricted its use to three hours daily, and utilized a minimal flexion angle. These modifications ultimately proved to be ineffective, as evidenced by multiple studies conducted by prestigious hospitals.
Since its inception, various CPM protocols have been implemented, but none have adhered to Salter’s original principles. These protocols have generally involved limited motion (due to inadequate pain control and apprehensions about wound dehiscence), discontinuous use (only a few hours daily), and delayed implementation (starting one day post-operatively). As a result, these studies have accurately demonstrated that such CPM protocols are lacking in efficacy.
However, the issue does not lie with the CPM machine itself, but rather with the protocols employed. By leveraging modern opioid-sparing pain control techniques, closing the wound in full flexion (we invented the Genuflex closure), and utilizing a drain to remove fluid from the knee, the CPM machine can be effectively employed through the AVATAR protocol. This groundbreaking approach initiates CPM immediately after surgery, with the knee flexed to 120 degrees. The machine is then used to gently maintain full motion throughout the night and for an additional eight hours daily for two weeks.
The fundamental principle of the AVATAR protocol is both uncomplicated and logical: by preventing stiffness from the beginning, the knee is less likely to develop restrictive scar tissue. This method has demonstrated considerable success, reestablishing the potential of CPM in post-operative care for total knee replacement patients when implemented with an effective protocol.